
"My first pregnancy was a semi-average pregnancy, with morning sickness for a solid three months and the uncomfortableness we all feel when we are growing our tiny humans. It wasn't until after my 20 week ultrasound I started spotting, on and off, for almost six weeks until, while at work, my water broke. At twenty-five weeks pregnant, this first time mother called her doctor.
I raced to Abbotsford Regional Hospital where they tested the fluids and confirmed my worst fear, it was amniotic fluid. I was then transferred to Royal Columbian Hospital (RCH), where they have the staff and equipment that would be required to help my baby and I survive this. I remained at RCH for the next two weeks, going into labour three times, back and forth to labour and delivery.
On June 24, 2021, I delivered my baby girl via emergency C-section. I didn't hear her crying. They reassured me she was ok, she needed a c-pap machine to help her breathe, but she was ok.
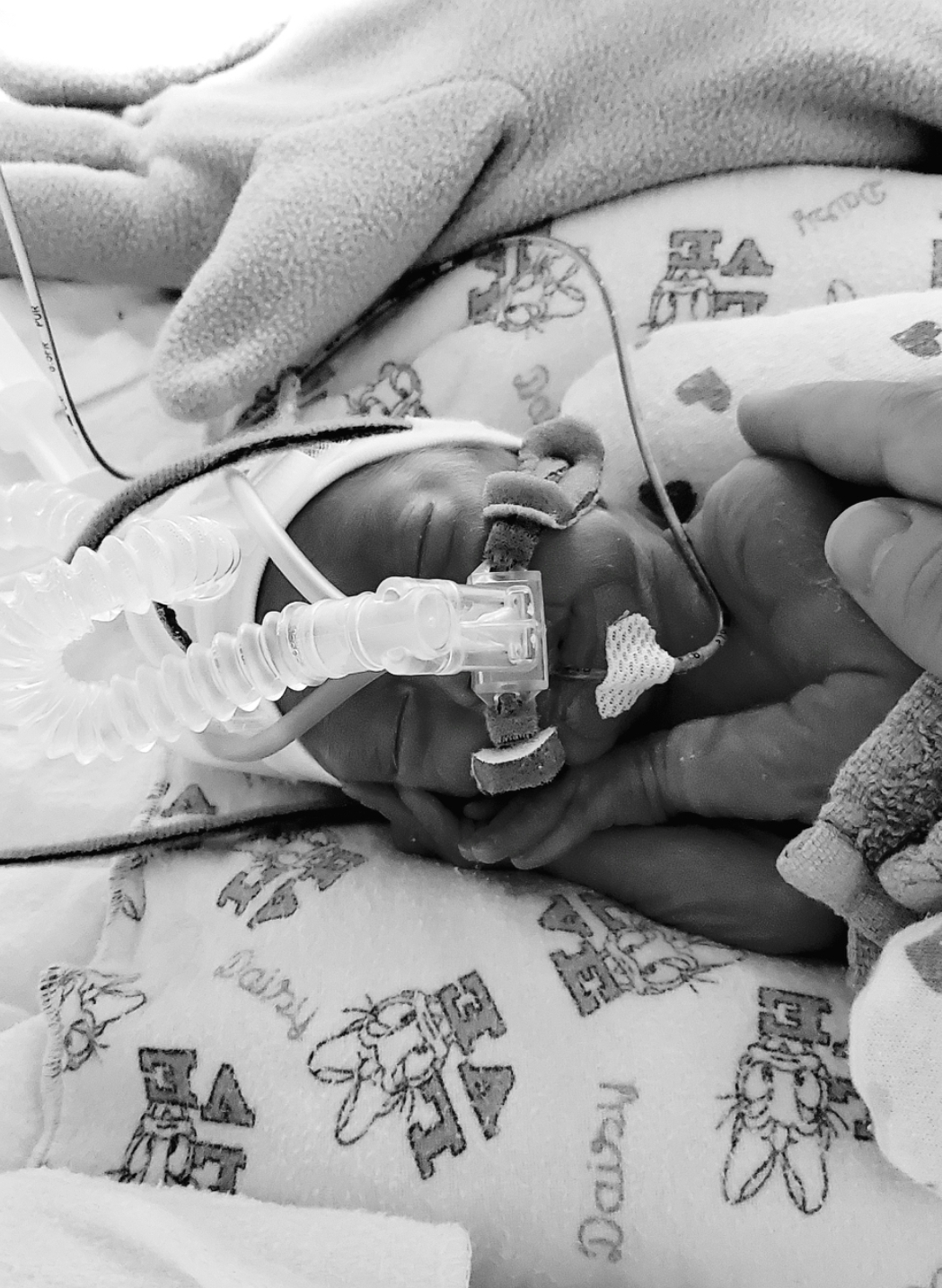
The next day, I got to hold her for 45 minutes, skin to skin. I had never seen such a tiny baby, or imagined I would ever hold something so fragile and beautiful. That was the start of our 79 days of life in the Neonatal Intensive Care Unit (NICU).
I thankfully was able to pump and start producing enough milk for my daughter on the second day. I believe she had donor milk for a couple of feeds to bridge the gap until my milk was enough. From that day on I pumped eight times per day for 15 minute pumps, and became an over producer. We bought a six-foot deep freezer and filled it over three months.
While I was able to provide my daughter with enough milk in the hospital, I was unable to breastfeed her since she was on a CPAP machine for seven weeks and was tube feed, orally and then nasally. I was thankful when we could start breastfeeding. I cut my pumping back and started our beautiful tradition of feeding together.
I know that this is my silver lining, that we could have a bit of normalcy and successfully breastfeed after all the tumultuousness that was our beginning. I know that not everyone is as lucky with that aspect, I watched mums struggle with pumping, producing or breastfeeding in the NICU. I was approached by many nurses and doctors about possibly of becoming a milk donor. I, of course, was interested.
I watched first hand as the tiniest humans benefited from this liquid gold. Not just benefiting, surviving because of it. I can honestly say, I had never known anyone else who had donated milk before.

I don't think I would have known to donate had I not given birth to a micro-preemie. I think that another silver lining to going through everything I went through is that in total, I was able to donate over 101 litres of milk to the milk bank (Lisa's "milk fridge" pictured to left). I know that my milk will not just help those babies, but save their lives.
Babies born, especially before 30 weeks, have to use their digestive systems too early. Formulas can be too hard on them, it can increase risks such as necrotizing enterocolitis, which is an intestinal disease and can cause death in premature babies. Our breast milk can save them. It broke my heart to hear how low the milk bank was on milk. I was informed that they had to make decisions on which babies were the most in need or earliest gestation for giving breast milk. I hope that in any future pregnancies I am able to donate again. I hope by sharing my story, I might reach some women and touch them enough to give the gift of their precious milk. You would be helping so many tiny local babies and their families. It is one of the most important things I have done in my life.

Lastly, I have a healthy, beautiful, intelligent, active almost two year old, Everly. I am so thankful that we beat so many odds that we faced. I think part of that is because of all that skin-to-skin, love and breast milk."
Less than one per cent of parents who gave birth in 2022 in B.C. donated to the provincial milk bank. Human milk has antibodies and immune factors that help protect babies from short- and long-term illnesses.
The BC Provincial Milk Bank serves all 14 Neonatal Intensive Care Units in the province and three additional B.C. hospitals have requested donor milk – Penticton Regional Hospital, Vernon General Hospital and Terrace Hospital.
The Provincial Milk Bank currently has less than an average month's supply and needs several months to meet upswings in demand as well as the fluctuation in donations. Every week the Milk Bank must turn down requests due to lack of supply.
Milk donors are healthy women who have delivered within the past 18 months and have more milk than they need.
Before attempting to drop off milk to any of the 28 milk collection depots across the province, potential donors must complete the screening process and call the depot they plan to use to confirm times and location for drop off.
Prospective donors can get information on milk donation on the
BC Women's website or by calling 604-875-3743.

